A rapidly growing intraoral lesion
A case study looking at a patient who presented with a long-standing swelling which was diagnosed as non-malignant peripheral odontogenic fibroma
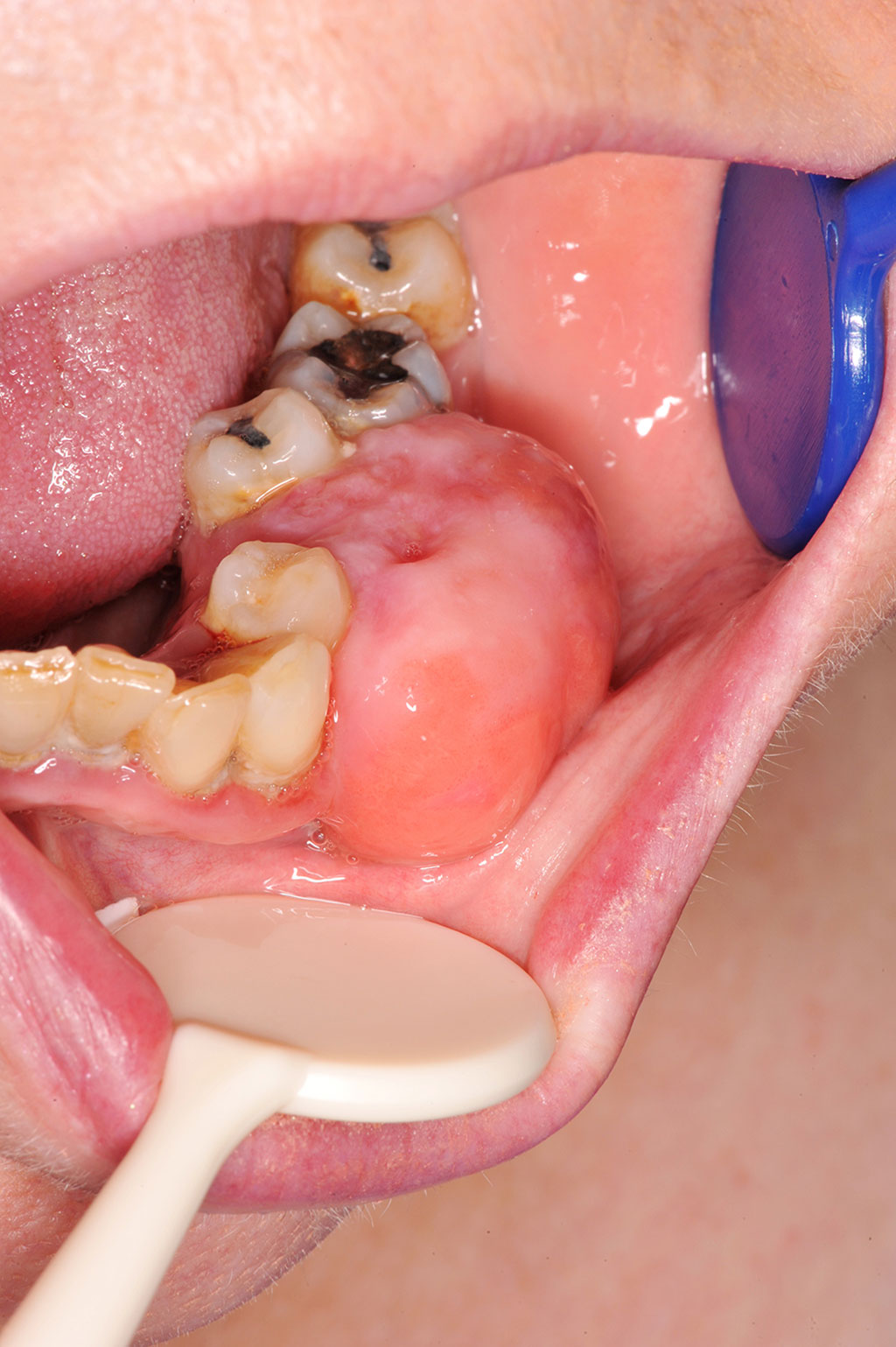
FIGURE 1: Pre-operative image of the lump
Gingival swellings are one of the most frequently encountered lesions in the oral cavity 1. Many different conditions can present as swellings, which in some cases can make diagnosis difficult. These can range from the benign un-concerning fibro-epithelial polyps to potentially life threatening malignant lesions such as squamous cell carcinomas.
Peripheral odontogenic tumours are a group of benign rare neoplasms that occur in the mouth 2. Peripheral odontogenic fibroma is the most common type of peripheral odontogenic tumour 3,4 and presents as a benign, slow-growing, exophytic growth of soft tissue usually involving the gingiva.
We present a case of a peripheral odontogenic fibroma mimicking common gingival swellings. The article aims to discuss a systematic approach to managing this case as well as highlighting other possible differential diagnoses. Table 1 provides an overview of swellings affecting the oral mucosa that may aid diagnosis.
An open mind should always be advised when managing many oral medicine/surgery cases. The oral cavity is a dynamic environment
Clinical case
A 62-year-old woman presented with a rapid increase in size of a long-standing swelling (Fig 1) affecting the lower left alveolus, which had been present for approximately six months. There was no associated pain or paraesthesia. Medically she had a diagnosis of atrial fibrillation, valvular heart disease and vertigo, which were managed appropriately. This included warfarin for her atrial fibrillation.
She was an ex-smoker of approximately 15 years and had occasional alcohol.
Extra oral examination revealed asymmetry of the left mandible. There was no lymphadenopathy. Intraorally the patient was partially dentate, had poor oral hygiene and clinical and radiological evidence of periodontal disease (Fig 2).
A large 2-3cm swelling was noted involving the lower left alveolus in the premolar region. Both the lower left first and second premolar were grade II mobile. The swelling was firm to palpate, fixed and with normal overlying mucosa.
Differential diagnosis
There are many causes of intraoral swellings and use of a surgical sieve approach provides a structured list of aetiological groups for systematically identifying potential causes of a presentation. These have been summarised in Table 1.
Management and outcome
Due to the sudden increase in the size of the swelling, urgent mapping biopsies of the lesion were taken. This confirmed an initial diagnosis of fibro-epithelial hyperplasia with no evidence of malignancy.
The patient was referred to the oral surgery department for removal of the residual swelling and the periodontal involved lower left premolar teeth. This was undertaken in the day procedure unit under local anaesthesia. Prior to undertaking surgery a pre-operative INR (2.12) test was carried out. The swelling and lower left premolar teeth were successfully removed under local anaesthetic. Haemostasis was achieved with cautery and the surgical site was dressed with both BIP (bismuth subnitrate, iodoform and paraffin paste impregnated gauze) packing and a suck-down vacuum splint for the first 24 to 48 hours.
At review one month post-surgery, the excision site was healing satisfactorily (See Fig 3). The final histopathology confirmed a diagnosis of a peripheral odontogenic fibroma. The patient will be reviewed on a three to six-month basis to monitor for recurrence. Further surgery may be required in the future.
- FIGURE 2: Image one month following excision
- FIGURE 3 : Orthopantomogram
Discussion
Peripheral odontogenic fibroma is the most common peripheral odontogenic tumour followed by the ameloblastoma and calcifying odontogenic tumour 3, 4. The most common location is the attached gingiva, usually in the molar/premolar area with even distribution between the jaws 5.
Peripheral odontogenic fibroma is an uncommon, benign, focal unencapsulated exophytic gingival mass, composed of fibrous connective tissue derived from mesenchymal origin 6. It may be pedunculated or sessile, red or pink, usually with a smooth surface and in some cases the overlying mucosa may be ulcerated. The lesion is usually firm to palpation, non-tender and could be mistaken for other more common exophytic gingival lesions, such as fibrous hyperplasia, pyogenic granuloma, or peripheral giant cell granuloma.
In the case above, the patient had been referred with a suspected oral cancer due to the rapid increase in size of a pre-existing swelling. During examination and periodontal probing, poor oral hygiene and periodontal disease could be justified for the possible cause of mobility of the premolars. An orthopantomogram radiograph did confirm bone loss consistent with periodontal disease. However, there was no periapical or bony pathology suggestive of a possible cystic, giant cell or aggressive lesion.
Due to the history of a rapid increase in swelling urgent mapping incisional biopsies were undertaken to give a better histological representation of the swelling. On the basis of this malignancy was excluded. A planned excision was arranged due to the size of the swelling and the patient’s complex medical history.
| Normal Anatomy |
|
| Developmental |
|
| Inflammatory |
|
| Traumatic |
|
| Neoplasms |
|
| Fibro-osseous |
|
| Hormonal |
|
| Metabolic |
|
| Drugs |
|
| Allergies |
|
| Viral |
|
Table 1: Main conditions which may present as swellings or lumps in the mouth
Conclusion
An open mind should always be advised when managing many oral medicine/surgery cases. Many gingival lumps and swellings have similar clinical presentations and may mimic that of something more sinister. The oral cavity is a dynamic environment. This, alongside ever more complex medical histories, presents the general dental practitioner with a puzzle of information.
Despite a myriad of aetiologies, gingival swellings and lumps can often be diagnosed by a careful history. Simple factors such as presence of local irritants such as calculus could be a primary cause. By carrying out routine full head, neck and intraoral examinations and managing plaque control potential development of lesions
may be prevented.
Should further management such as biopsy, biochemistry or histological examination be required, it is important that the clinician makes an appropriate referral, providing all the essential information to enable effective, efficient and safe management of the patient.
About the author
Colm Hicks, BcHD, MFDS RCSEd; Amanda Willis, BDS, BMedSci (Hons), MMedSci PHD, MJDF RCSEng, PGCE, FDS (OM) RCPS(Glasg); John Marley, BSc BDS, PhD, FDS (OS)RCS Eng, FFDRCSI.
The authors would like to acknowledge Dr Seamus Napier, consultant oral pathology for carrying out the histopathology for this case.
References
1. Kannan S, Thapasum A, Suresh N, Muthusamy S, Chandrasekaran B. Localised Gingival Overgrowth – Differential Diagnosis for Dental Practitioners. Dental Update 2014; 41: 698–706.
2. Manor Y, Mardinger O, Katz J, Taicher S, Hirshberg A. Peripheral odontogenic tumours – differential diagnosis in gingival lesions. International Journal Oral Maxillofacial Surgery. 2004; 33: 268–273.
3. Ide F, Obara K, Mishima K, et al. Peripheral odontogenic tumor: A clinicopathologic study of 30 cases. General features and hamartomatous lesions. Journal Oral Pathology Medicine 2005; 34:552.
4. Buchner A, Merrell PW, Carpenter WM. Relative frequency of peripheral odontogenic tumors: A study of 45 new cases and comparison with studies from the literature. Journal Oral Pathology Medicine 2006; 35:385.
5. Kenny JN, Kaugars GE, Abbey LM. Comparison between the peripheral ossifying fibroma and peripheral odontogenic fibroma. Journal of Oral and Maxillofacial Surgery 1989; 47(4): 378-382.
6. Savage N W, Daly C G. Gingival enlargements and localised gingival overgrowths. Australian Dental Journal 2010; 55: 55-60.
7. Felix H D, Luker J, Scully C Prof. Oral Medicine:11. Lumps and Swellings: Mouth. Dental Update 2013; 40: 683 – 687.
8. Saravana GHL. Oral pyogenic granuloma: a review of 137 cases. British Journal of Maxillofacial surgery 2009; 47:318 -319.
9. Motamedi MH, Eshghyar N, Jafari SM, et al. Peripheral and giant cell granulomas of the jaws: a demographic study. Oral Surgery Oral Medicine Oral Pathology Oral Radiology Endodontolgy 2007; 103: 39-43.
10. Walsh T, Liu JLY, Brocklehurst P, Glenny AM, Lingen M, Kerr AR, Ogden G, Warnakulasuriya S, Scully C. Clinical assessment to screen for the detection
of oral cavity cancer and potentially malignant disorders in apparently healthy adults. Cochrane Database of Systematic Reviews 2013, Issue 11.
11. Smittenaar CR, Petersen KA, Stewart K, Moitt N. Cancer incidence and mortality projections in the UK until 2035. Br J Cancer. 2016 Oct 25; 115(9): 1147–1155.
12. National Institute for health care and excellence. Suspected cancer: recognition and referral – NICE Guideline NG12. 2015 (last updated July 2017) available online www.nice.org.uk/guidance/ng12/resources/suspected-cancer-recognition-and-referral-pdf-1837268071621 [last accessed January 18, 2018]
.
13. Healthcare improvement Scotland. Scottish referral guidelines for suspected cancer 2013 (updated in August 2014) available online www.healthcareimprovementscotland.org/our_work/cancer_care_ improvement/programme_resources/scottish_referral_guidelines.aspx [last accessed 18 January, 2018].
14. Agrawal AA: Gingival enlargements. Differential diagnosis and review of literature. World Journal of Clinical Cases 2015; 16: 3(9): 779-788.
15. Hallimon WW, Rossmann JA. The role of drugs in the pathogenesis of gingival overgrowth. A collective review of current concepts. Periodontology 2000; 21: 176-196.
16. Sculley C, Porter S. Orofacial Disease. Update for the Dental Clinical Team: 5. Lumps and Swellings. Dental Update 1999; 26: 214-217.
Verifiable CPD Questions
Aims and Objectives:
To discuss the signs and symptoms associated with a peripheral odontogenic fibroma
To inform readers of the management of lesions such as a peripheral odontogenic fibroma
To inform readers of other potential differential diagnoses for similar intraoral presentations.
LEARNING OUTCOMES:
Readers will be able to gain an accurate history associated with such intraoral lesions
Readers will be able to make a differential diagnosis for similar intraoral swellings.
Readers will be able to inform their patients better of potential diagnoses and the future management of such intraoral swellings.
How to verify your CPD
Go online to https://https://https://https://sdmag.wpengine.com and click
on the CPD tab to access all our CPD
Q&As and certificates


Comments are closed here.