Safeguarding and child protection for the dental team
Do you know what to do, or who to contact, if you or a member of your team raises concerns about a paediatric patient?
I’ve been teaching in the area of child protection and dentistry for approximately eight years and completed a masters by research in 2013 on Oral Disease in Vulnerable Children and the Dentist’s Role in Child Protection1. I’m now doing a PhD looking at what is involved in the decision by dental team members to refer suspected cases and how serious game methodology might support this context.
What is clear to me is that often decisions in this area are difficult and uncomfortable to make, so this article looks at what is expected of us as members of the dental team (whether we are dentists, dental nurses, therapists or technicians) and what this means from a practical point of view in our daily working lives.
The General Dental Council states that all members of the dental team “must raise any concerns you may have about the possible abuse or neglect of children” and “must know who to contact for further advice and how to refer concerns to an appropriate authority”2. They also state “you must find out about local procedures for the protection of children” and “you must follow these procedures if you suspect a child or vulnerable adult might be at risk because of abuse or neglect”2.
I have had to look at statements from dental team members when something awful has happened to one of their paediatric patients, and so often there have been warning signs
These wide-ranging statements mainly cover child protection (defined as activities undertaken to protect specific children who are suffering, or are at risk of suffering significant harm) but also bring in elements of safeguarding (defined as measures taken to minimise the risk of harm to all children).
From a practical point of view, there is the need to identify what your concerns are. This could be anything from unexplained (or inadequately explained) injuries, concerns about dental neglect, concerns about general neglect, a general lack of engagement with dental services to witnessing a child being physically abused in your waiting room or surgery. It is the vast spectrum of these concerns which make it difficult to provide what so many people ask for – a step-by-step guide for any conceivable situation – because there are so many different situations that could present themselves.
Some health boards have produced flowcharts for dental teams to follow and there is also a summary flowchart available on the Child Protection and the Dental Team website which are very helpful3. For some of these situations, the dental team members that I have been privileged to speak to (during my research and teaching) find the decision of what to do next straightforward, but for other situations it is more difficult.
It has already been well documented that there remains a 26 per cent gap between the proportion of general dental practitioners who have suspected child abuse or neglect in one or more of their paediatric patients (37 per cent) and the proportion that have referred suspected cases (11 per cent)4. Quantitative methods have consistently shown that the gap between dentists who suspect and refer in Scotland is affected by lack of certainty of the diagnosis, fear of violence to the child, fear of consequences to the child from statutory agencies, lack of knowledge of referral procedures, fear of litigation, fear of violence to the general dental practitioner and concerns of impact on dental practices4, 5.
So, let’s explore four of the most common things I’m asked about and hopefully it will be helpful to all of the team.
1. The child with caries whose family don’t engage with services
I’m asked about this situation a lot, probably because it is a common occurrence. We know caries is still common in children and statistics say 94 per cent of children in Scotland are registered with a general dental practitioner, with 85 per cent having seen their dentist in at least the last two years6. Perhaps a dentist has referred a patient for extractions under general anaesthetic but the patient is never taken to the assessment appointment and the dentist gets a letter back from the public dental service or the hospital dental service discharging them back to their care because they’ve not managed to see them.
Or perhaps it is a family that come for their check-ups but don’t bring the children back to have their treatment completed, or ones who repeatedly cancel, or don’t book check-ups when they get their reminder letters and the dental teams only end up seeing them sporadically. Or it may be children who have required extractions under general anaesthesia for removal of all their primary teeth but then don’t come back until they are aged seven or so and now have unrestorable caries in all their permanent molars.
These situations are difficult and all of them are examples of dental neglect, which is defined by the British Society of Paediatric Dentistry as “the persistent failure to meet a child’s basic oral health needs, likely to result in the serious impairment of a child’s oral or general health or development”7. Although dental caries is still common in children, signs such as failing to complete courses of dental treatment, failing to listen and act on preventive advice given by dental teams, children returning in pain repeatedly, children requiring repeated general anaesthetics due to dental issues or children who are repeatedly not brought to their dental appointments, are all concerning patterns of behaviour which are likely to result in the impairment of a child’s oral or general health or development7,8.
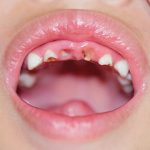
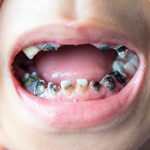
Untreated dental caries may be one of the first signs of child abuse or neglect9. Neglect should be considered if parents have access to, but persistently fail to obtain treatment for their child’s tooth decay10. Research also suggests that abused/neglected children are more likely to have untreated decayed teeth, significantly more dental plaque and gingival inflammation than non-abused/non-neglected children11–13.
Many practitioners whom I have spoken to then say: “Well if I have to refer every patient like that, I would be referring at least 60 per cent or more of my paediatric cohort!” This really depends on what practitioners mean by the term ‘refer’. All of these situations do require some action to be taken, but not all will necessitate an immediate referral to social work. There is very sensible advice given for this type of scenario in Child Protection and the Dental Team (CPDT) which recommends a three-level response to concerns about dental neglect, namely preventive dental team management, preventive multi-agency management, child protection referral3.
Preventive dental team management involves “raising concerns with parents, offering support, setting targets, keeping records and monitoring progress. The initial focus should be on relief of pain accompanied by preventive care. In order to overcome problems of poor attendance, dental treatment planning should be realistic and achievable and negotiated with the family”3. This is often all that is required and, in reality, is probably what most dental teams do on a day-to-day basis (although there is no evidence from research to prove this is the case).
Fully implementing a preventive dental team management strategy can have impacts on a practice and those impacts will have to be discussed as a team, for example deciding who will deal with contacting the family if agreed appointments are cancelled or missed. The CPDT website gives an example of how it might be put into practice3. The areas where research has suggested dental teams could improve upon are ‘setting targets’ and ‘monitoring progress’14. If this level of response to the concerns is not working or there is a breakdown of communication or the child/family has more complex needs then preventive multi-agency management may be more appropriate.
Preventive multi-agency management involves liaising with other professionals who might be involved with the family. Examples of other professionals could include the health visitor (for pre-school children), the general medical practitioner, the child’s social worker (if they already have one) or the child’s named person. The aim of this liaison is “to see if concerns are shared and to clarify what further steps are needed”3. There is a sample letter to a health visitor freely available on the CPDT website which can be used to assist with multi-agency working for children under five years old3.
A joint plan of action should be agreed (for example as a dental practice we will arrange appointments on these dates and the child’s social worker will facilitate attendance, or the health visitor will arrange a home visit by a dental health support worker to facilitate registration and attendance at our dental practice). A date should be specified for review of the action plan so that it can be checked that progress is being made.
If there is any point in the processes above where things begin to deteriorate, or if it is felt at any time that the child is at risk of suffering significant harm (this can include things like a child being in pain for more than a couple of days due to toothache and this is happening on more than one occasion), then any member of the dental team can make a child protection referral. Some dental team members struggle to work out when things become significant. A good rule of thumb can be that if you wouldn’t let children in your own circle of family or friends go through it, then it is probably significant.
Child protection referrals should be made according to the local procedures of where you work. In Scotland, a child protection referral is made either to the police or local children’s social work team (referrals can also be made to the Children’s Reporter but follow your local guidelines). If you do not already know your local contact numbers you can, currently, find them out by visiting www.withscotland.org/public-local-councils and typing in the postcode of the child you are concerned about. (Please note: This website address is likely to change in the future as WithScotland no longer exists, but many of their functions have been taken over by the new Centre for Child Wellbeing and Protection www.stir.ac.uk/ccwp/)
- Caries in children can be evidence of neglect at home
2. How do I make a child protection referral?
The majority of child protection referrals will involve a telephone call to your local social work office (Children and Families office ideally but in many areas in Scotland you will go through Social Care Direct) in the first instance explaining your concerns and stating you wish to make a child protection referral. Write down the names and job titles of everyone you speak to. The telephone referral should then be followed up in writing normally within 48 hours. This may involve completion of a shared referral form, or notification of concerns form (same form just different names), or similar, with one copy going into the child’s dental notes, one copy sent to the social work office that you spoke to on the phone, and, depending on your local procedures, another copy may be sent to your local child protection unit (CPU) or similar (or you may just have to notify your CPU by email or phone).
3. Will the family know I’ve referred them?
The short answer to this is that they might. In most situations it is best practice to tell the family what your concerns are and why you are referring them to social services but there will, of course, be some situations where the family don’t know, either because you can’t get in contact with them or you may believe that you would put the child in more danger if the family were aware of the referral.
You can refer anonymously but, bear in mind that if the concerns you have are related to non-attendance with you or concerns about something dental, then even if you refer anonymously the family will, probably, be able to work out where the referral came from so it is a much better situation if you have informed them the referral is being made.
4. I’m worried about how the family will react
Many dental professionals assume telling a family you are going to contact social work will be bad news, but for some families it will be the first time anyone has actually offered them any help. As members of the dental team, we quite often have to break bad news to our patients (e.g. “I’m sorry I can’t save the tooth, it needs to be extracted”). Being concerned is a natural human response but it is helpful to think through all the reactions that you would be worried about and how, as a team, your practice will manage them.
For example, if the family are angry and choose to de-register from your practice, you can’t always prevent that from happening but you would want to pass that information on to the other agencies involved such as the social work office you referred to. I suggest being quite clear in your practice about what your professional responsibilities are and having posters or information up in waiting areas promoting that you take the safeguarding of children and vulnerable adults seriously.
Many dental team members have told me they are worried that as they live in a small town that word will spread, or their own children will be targeted at school or they will be threatened by the families involved. My advice is that if you are threatened, inform the police and relevant social work office involved. If your own children get picked on because of rumours, approach the school as you would do about any episode of bullying your child may experience and talk to your child about the nature of your job (e.g. “You know mummy/daddy is a dentist/dental nurse/practice manager and looks after people’s teeth, but I also have a responsibility to make sure the children that I see at work are alright and are being looked after properly”). If your practice gets branded as “the ones who call social work”, take this as a good thing as it means you are actively looking out for and promoting the welfare of your paediatric patients. There are many experts out there who can give advice on how to use it as a
‘practice builder’.
Conclusion
Ultimately, it is not only our professional responsibility, but also an ethical responsibility to protect and safeguard those in society who can’t do it for themselves. Doing nothing when you have a concern is never an option – you would probably continue to worry and you cannot predict what the impact on the child would be.
Unfortunately, I have had to look at statements from dental team members when something awful has happened to one of their paediatric patients, and so often there have been warning signs (e.g. multiple missed appointments, failure to complete treatment) but the dental teams did not record or raise any concerns. Clearly I have the benefit of hindsight and experience but my hope is that as more dental teams think about and practise looking out for the wellbeing of their paediatric patients, then perhaps I’ll see fewer awful things happening. Or, if they are still happening, I’ll see real evidence that the dental teams involved did everything they could to help the child.
About the author
Christine Park is a senior clinical university teacher at Glasgow Dental Hospital and School, and honorary consultant in paediatric dentistry at NHS Greater Glasgow and Clyde.

References
1. Harris CM. Oral disease in vulnerable children and the dentist’s role in child protection [MSc Thesis] Glasgow: University of Glasgow; 2013. Available at: http://theses.gla.ac.uk/4150/1/2013harrismsc.pdf.pdf Accessed 03/08/2017
2. General Dental Council. Standards for the Dental Team. Guidance on Child Protection and Vulnerable Adults. GDC; 2013. Available at www.gdc-uk.org/professionals/standards/team Accessed 03/08/2017
3. Harris J, Sidebotham P, Welbury R et al. Child protection and the dental team. An introduction to safeguarding children in dental practice. Sheffield: Committee of Postgraduate Dental Deans and Directors, 2006. Available at: bda.org/childprotection Accessed 03/08/2017
4. Harris CM, Welbury, R, Cairns, AM. The Scottish dental practitioner’s role in managing child abuse and neglect. Br Dent J 2013; 214(E24):1–5. Available at: dx.doi.org/10.1038/sj.bdj.2013.435 Accessed 03/08/2017
5. Cairns AM, Mok JYQ, Welbury RR. The dental practitioner and child protection in Scotland. Br Dent J 2005; 199(8):517–520; discussion 512; quiz 530–531.
6. ISD Scotland. Dental Statistics – NHS Registration and Participation. A National Statistics Publication for Scotland; 2017. Available at:
www.isdscotland.org/Health-Topics/Dental-Care/Publications/2017-01-24/2017-01-24-Dental-Report.pdf?49161928893 Accessed 03/08/2017
7. Harris JC, Balmer RC, Sidebotham PD. British Society of Paediatric Dentistry: a policy document on dental neglect in children. Int J Paediatr Dent 2009. Available at: http://bspd.co.uk/Portals/0/Public/Files/PolicyStatements/Dental%20Neglect%20In%20Children.pdf Accessed 03/08/2017
8. Balmer R, Gibson E, Harris J. Understanding child neglect. Current perspectives in dentistry. Prim Dent Care 2010; 17: 105–109.
9. Blumberg ML, Kunken FR. The dentist’s involvement with child abuse.
NY State Dent J 1981; 47:65–69.
10. National Collaborating Centre for Women’s and Children’s Health (2009). When to suspect child maltreatment: full guidance. Clinical Guideline 89. National Institute for Health and Clinical Excellence. Royal College of Obstetricians and Gynaecologists: London. Available at www.nice.org.uk/guidance/cg89/evidence/cg89-when-to-suspect-child-maltreatment-full-guideline2 Accessed 03/08/2017
11. Greene PE, Chisick MC, Aaron GR. A comparison of oral health status and need for dental care between abused/neglected children and non-abused/non-neglected children. Pediatr Dent 1994;16:41-45
12. Valencia-Rojas N, Lawrence HP, Goodman D. Prevalence of early childhood caries in a population of children with history of maltreatment. J Public Health Dent 2008;68(2):94-101
13. Montecchi PP, Di Trani M, Sarzi Amadè D, et al. The dentist’s role in recognizing childhood abuses: study on the dental health of children victims of abuse and witnesses to violence. Eur J Paediatr Dent 2009; 10(4):185-187.
14. Harris JC, Elcock C, Sidebotham PD, Welbury RR. Safeguarding children in dentistry: 2. Do paediatric dentists neglect child dental neglect? Br Dent J 2009;206: 465 – 470
Verifiable CPD Questions
Aims and objectives:
- To discuss some common concerns with regards to safeguarding and child protection in general dental practice
- To inform readers about various web resources such as Child Protection and The Dental Team and the WithScotland website that can provide further useful information
- To encourage dental teams to think through how they will handle reactions from families.
Learning outcomes:
- Readers will understand what the GDC expects of its registrants with regard to safeguarding of paediatric patients
- Readers will know what to do if they have concerns about a child with caries whose family don’t engage with dental services
- Readers will know how to make a child protection referral.


Comments are closed here.