Chronological vs biological age
When it comes to treating the ageing population, the best treatment might not be the most appropriate
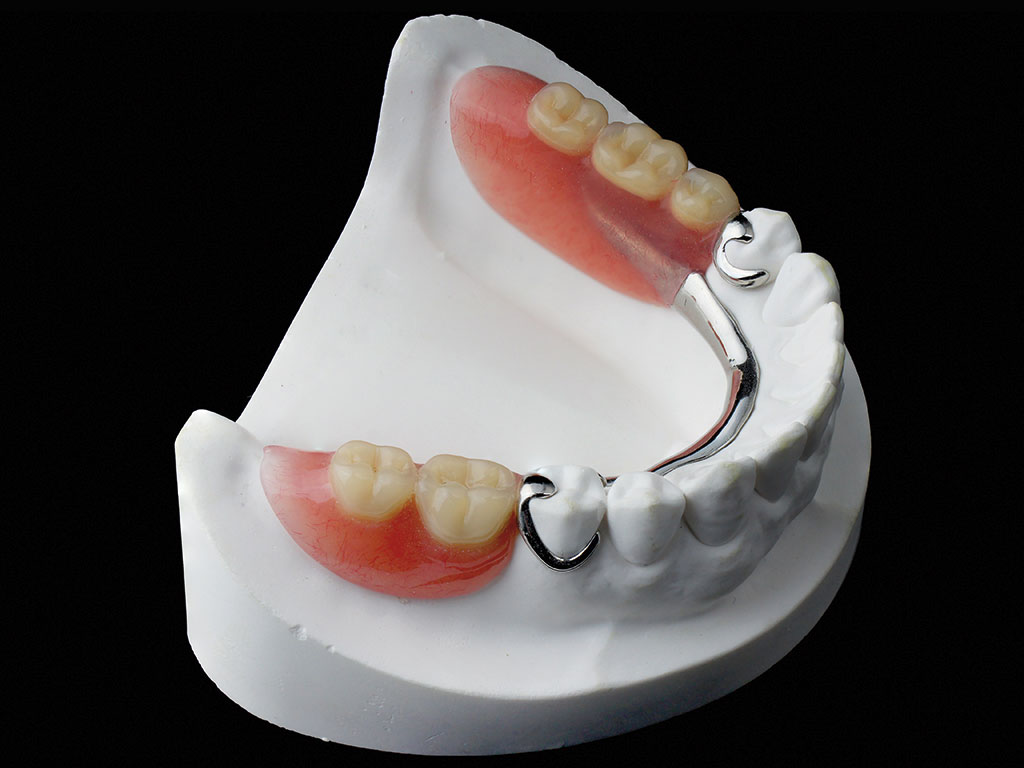
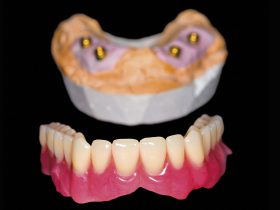
FIGURE 1 – Removable partial chrome cobalt denture
In 2013, 14 per cent of the world’s population was over 60 years of age. It is estimated that, by 2050, this figure will have increased to 19 per cent 1. However, as people age they develop more health conditions. Multimorbidity is the “presence of two or more diseases in one person” 2. Research indicates that, by 70 years of age, 63 per cent of people can expect to have developed two or more disorders 3.
Common chronic conditions in the elderly include cardiovascular disease, type 2 diabetes, depression, COPD and osteoarthritis. Multimorbidity has been shown to impact immune function greater than age alone 4.
These multiple chronic conditions can also result in polypharmacy where patients have to manage an increasing number of medications. In Europe, over half of the elderly population take more than six medications per day 5. This results in an increased risk of adverse drug events. Treatment plans for an elderly patient should be based on their individual risk factors, functional difficulties and preferences.
A growing elderly population increases the indications for partial removable dental prostheses and expands the indications for implant therapy. When considering implant surgery in elderly patients, pre-operative medical fitness is more important than chronological age 6.
The standard of care in geriatric patients has to be adapted to the patient’s motivation, medical condition and socio-economic circumstances. Oral health can significantly affect an elderly patient’s nutritional intake. It has been found that complete denture wearers have thinner masseter muscles whereas implant retained over-dentures lead to increased muscle thickness 7. Unlike most adults, a BMI >25 in elderly patients is associated with a reduced mortality. It is therefore important that elderly people can chew adequately to avoid restricted diets which offer lower nutritional values 8.
Medical consideration in elderly patients considering dental implant treatment
Cardiovascular diseases
These can be divided into atherosclerosis, hypertension, chronic heart failure and atrial fibrillation. A recent myocardial infarction, stroke and cardiovascular surgery is an absolute contraindication to implant surgery 9. Medical control of the disease is imperative prior to implant therapy. Patients with stent implantation after coronary artery disease usually have dual antiplatelet blood-thinning therapy to prevent clot formation.
Bleeding disorders
Bleeding can be prolonged in patients with haemophilia or those taking medication such as warfarin for anticoagulation. Current recommendations advise against modifying the anticoagulation provided the INR is <3.5. The exception may occur upon consultation with the patient’s medical team in cases of high volume bone grafting or extensive flaps. Splints can be used to manage expected bleeding.
The number of patients taking new oral anticoagulants such as dabigatran and rivaroxiban is increasing. New oral anticoagulants do not require monitoring, however, they lack a reversal agent. It is important that dentists follow the most recent guidelines regarding the management of these patients especially when considering invasive implant surgery 10.
Poorly controlled diabetes mellitus
This can result in delayed wound healing, an impaired response to infection and susceptibility to periodontal disease. Dentists should check their patient’s HbA1C (glycosylated haemoglobin) prior to implant placement. Implant and bone augmentation surgery in an uncontrolled diabetic can lead to serious wound healing complications.
- FIGURE 1 – Removable partial chrome cobalt denture
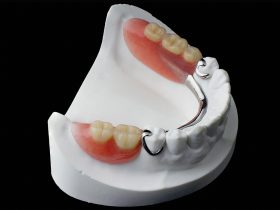
- FIGURE 2 – Extended implant fixed partial denture
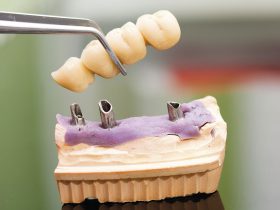
- FIGURE 3 – Lower implant over-denture bar
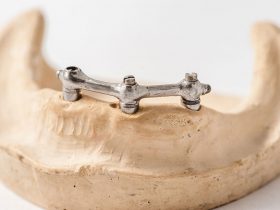
- FIGURE 4 – Implant-retained over-denture
Osteoporosis
A decrease in bone mass and bone density increases the risk of fracture. Oral bisphosphonates reduce osteoclast function increasing the risk of bisphosphonate-related osteonecrosis of the jaw. Oral bisphosphonates are a potential risk factor for osteonecrosis of the jaw but not for implant success and survival 11.
Chronic obstructive pulmonary disease
Chronic bronchitis and emphysema result in a chronic cough, sputum production and shortness of breath. Special consideration needs to be given to the type of local anaesthetic administered. It is recommended that the maximum dose of local anaesthetic be halved in patients >65 due to reduced liver function 12. Also dentists should be mindful of the risk of adrenal insufficiency in elderly patients taking long-term steroids.
Psychological conditions
Depression is common among the elderly population. At the age of 90, three out of four patients have a diagnosis of dementia 13.
Treatment planning options
Shortened dental arch concept
The shortened dental arch is where 10 upper teeth oppose 10 lower teeth 14. Dentists can reduce the biological risks for the patient and avoid problems of low acceptance by providing this treatment option 15. Gerritsen et al concluded that a shortened dental arch can last for 30 years and that there is no recommendation for adding a partial denture. McKenna et al also examined the shortened dental arch concept in 89 patients who were >65 years old. His results demonstrated a better oral health related quality of life score in patients with a shortened dental arch compared with those wearing removable partial dentures 16.
Removable partial dentures (RPD)
This is an economical prosthodontic solution involving sound abutment teeth for increased retention. It helps maintain teeth of strategic value if implants are not an option 17. The prosthetic flange can also maintain facial fullness. However, abutment teeth for removable partial dentures are high risk for both caries and periodontal disease.
Prognostic factors for partial RPD abutments include 18:
- Crown-root ratio
- Root canal treatment
- Periodontal pocket depth
- Type of abutment – multi-rooted maxillary molars can make for unfavourable abutments
- Occlusal support and function of the abutment tooth.
Partial removable dentures with implants
Conventional dentures have limitations as oral function can decline with age. Old age is not a contraindication for dental implant treatment however; some medical conditions can increase their risk of failure. It is the degree of systemic disease control that is important rather than the nature of the disorder itself. Dentists should consider the American Society of Anesthesiology’s (ASA) Classification. The ASA restricts dental implants to ASA 1 and 2 patients. Dental implant placement may be undertaken in some very carefully considered ASA 3 cases.
In comparison with conventional dentures, implant over-dentures have the advantage of slowing peri-implant bone resorption and preventing bone atrophy 19. There is also a significant improvement in chewing ability with two lower implant supported over-dentures as a result of improved muscle co-ordination. Implants increase support, retention and can improve the aesthetic outcome of dentures by avoiding the use of clasps which results in greater patient satisfaction.
Strategic implant positioning can also help convert a Class I and Class II Kennedy arch into a Kennedy Class III configuration following the extraction of a hopeless abutment. This improves the elderly patient’s ability to eat harder food when compared with a conventional complete denture. This encourages elderly patients to eat a more diverse diet, which not only boosts their nutritional intake, but also enables them when socialising to finish their meals at the same time as family and friends 20.
Implant-supported over-dentures are also associated with psychological benefits such as improved social interactions and better self-confidence. Wismeijer et al examined patient satisfaction among 36 conventional and implant assisted partial denture wearers 21. The results showed a significant improvement in patient satisfaction with support of healing caps on implants as opposed to the conventional partial removable denture by itself. There was an even greater improvement in patient satisfaction when ball anchors were attached to the implants for retention.
In cases where patients are fully edentulous the recommended configurations are:
- Four or more implants in maxilla
- Two or more implants in mandible.
Removable options for the fully edentulous patient
The McGill Consensus statement on over-dentures recommends that “a two-implant over-denture should become the first choice of treatment for the edentulous mandible” 22. Implant-retained over-denture designs should be easy to clean, repair and also to re-activate retention. Long-term results suggest that a mandibular over-denture retained by two implants with a single bar may be the best treatment strategy for edentulous patients with an
atrophic ridge.
A bar can remove pressure from the tissue 23. There appears to be no influence with regards to the length of the cantilever arm (up to 12mm) and crestal bone loss 24. There is also good evidence to support the use of four implants with single retentive elements in the maxilla with a conventional loading protocol 25.
Combination syndrome
Two implants have an axis of rotation meaning that forces on the posterior ridge are higher than if the patient had a complete denture. Anterior flabby ridges and more posterior ridge loss can result from two implants necessitating more frequent denture relining in the upper jaw 26.
Short and reduced diameter implants
Short and reduced diameter implants are increasingly making dental implants possible in low and narrow alveolar ridges. They preserve bone and reduce the mouth opening requirements for an elderly patient. The surgery is less invasive and the need for augmentation procedures is eliminated, which results in less surgical morbidity.
The reduced complexity of the procedure also reduces the financial burden on the patient. Short and narrow implants make the reversible ‘backing off’ strategy easier if for instance a patient undergoing chemotherapy can no longer manage their dentures.
Implant configurations for Fixed Dental Prosthesis (FDP)
It is not necessary to replace every tooth that is missing in an elderly patient. Careful assessment is required when choosing the type and dimensions of implants. The minimal distance between teeth and implants must be respected and also bearing in mind the need for pink aesthetics. Short edentulous spaces that comprise of three missing teeth can normally be restored with two implants. Cantilevers help avoid bone augmentation procedures which can reduce the surgical morbidity for elderly patients.
Extended edentulous spaces have greater than three teeth missing. Implant positions are determined by the prosthodontic plan considering the number of teeth to be replaced, anatomical limitations and the bone volume present. When four teeth are missing in the anterior region, two implants and a FDP with a pontic or cantilever design can be utilised. When four teeth are missing posteriorly two to three implants are usually sufficient, utilising a one piece or segmented design.
An edentulous ridge can be restored with a one-piece FDP or three to four segmented FDPs. A full-arch one-piece FDP requires four to six implants. Utilising the shortened dental arch concept or cantilever units can help reduce the number of implants required for a FDP in the edentulous ridge. The implant sites should be evenly spaced if possible. Cantilevers can eliminate the need for a sinus augmentation procedure in the maxilla. Distal implants can also be straight or tilted to help avoid anatomical structures.
Full arch segmented FDP are indicated in certain cases where patients have gradually lost teeth or if segments need to be removed for periodic cleaning. Full arch segmented FDPs usually require more implants such as eight in the maxilla and six in the mandible. The implants can be strategically positioned to allow three to four short-span implant-supported FDP 27.
Conclusion
Dentists can provide life-changing treatment for patients of advanced age. Minimally invasive interventions with reduced healing times are recommended. Strategies for successful dental treatment for elderly patients must allow for frequent breaks, postural issues and increased chair time. Access and mobility issues can become barriers to care as patients become more reliant on others and experience reduced autonomy. It must be borne in mind that complications and prosthetic repairs are frequent 28.
Objective information should be clearly provided in writing and, where possible, with pictures. Declining cognitive function can affect a patient’s understanding of treatment, which raises the issue of valid consent. It is crucially important that patients have proven oral hygiene compliance. A prosthesis which is easy to manage and straightforward to clean will increase patient
acceptance 29. Neuroplasticitiy reduces in ageing patients making it difficult to develop new muscular patterns when adjusting to a denture.
Careful case selection is crucially important for patients advancing in age. It is important for dentists to address the patient’s specific concerns and to remember that the best treatment may not always be the most appropriate. Dentists must follow up on patients who have become institutionalised in order to implement a “back-off” strategy if necessary. Modifications that make denture management easier such as unscrewing an implant ball attachment and relining a denture can dramatically improve an elderly patient’s quality of life. The goal of treatment planning should allow for simple therapeutic step-back solutions if the patient enters a period of decline.
About the author
Dr Laura Fee graduated with an honours degree in dentistry from Trinity College, Dublin. During her studies, she was awarded the Costello medal for undergraduate research on cross-infection control procedures. She is a member of the Faculty of Dentistry at the Royal College of Surgeons and, in 2013, she completed the Certificate in Implant Dentistry with the Northumberland Institute of Oral Medicine and has since been awarded the Diploma in Implant Dentistry with the Royal College of Surgeons Edinburgh. Laura is currently completing the Certificate in Minor Oral Surgery with the Royal College of Surgeons, England. She has also been involved with undergraduate teaching in the School of Dentistry, Belfast where she has an honorary oral surgery contract.
References
- United Nations, Department of Economic and Social Affairs, Population Division (2013). World Population Ageing 2013
- Mercer et al Multimorbidity in primary care: developing the research agenda. Family Practice 2009 26(2):79-80
- Barnett et al Epidemiology of multimorbidity and implications for health care, research and medical education: a cross sectional study. The Lancet 2012:380:37-43
- Castle SC et al. Comorbidity is a Better Predictor or Impaired Immunity than Chronological Age in Older Adults. J Am Geriatr Soc. 53(9):1565-9
- Fialova et al. Potentially inappropriate medication use among elderly home care patients in Europe. JAMA. 2005; 293:1348-1358)
- Seymour DG, Vaz FG. A Prospective-Study of Elderly General Surgical Patients 2: Postoperative Complications. Age and Ageing 1989 Sept, 18(5): 316-26
- F Muller et al. Masseter muscle thickness, chewing efficiency and bite force in edentulous patients with fixed and removable implant-supported prostheses: a cross-sectional multicentre study. Clinical Oral Implants Research, 2012, vol.23, no. 2,p.144-50
- Weiss A et al. Body Mass Index is Inversely Related to Mortality in Elderly subjects. Journal of General Internal Medicine 23(1) 19-24(2007)
- Hwang D, Wang HL. Medical contraindications to implant therapy. Part 1. Absolute contraindications. Implant Dent 2006;15(4): 353-60
- O’Connell JE, Stassen LF. New oral anticoagulants and their implications for dental patients. J Ir Dent Assoc 2014 Jun-Jul;60(3):137-43
- Kumar MN, Honne T. Survival of dental implants in bisphosphonate users versus non-users: a systemic review. Eur J Prosthodont Restor Dent 2012 Dec; 20(4):159-62
- Daublander M, Muller R, Lipp MDW. The incidence of complications associated with local anesthesia in dentistry. Anesth Prog 1997;44:132-141
- Stone AA, Schwartz JE, Broderick JE, Deaton A. A snapshot of the age distribution of psychological well-being in the United States. Proc Natl Acad Sci USA 2010 107(22) 9985-90 – patients get happier as they age.
- Kayser AF. Shortened dental arch: a therapeutic concept in reduced dentitions and certain high-risk groups. Int J Periodontics Restorative Dent 1989;9(6):426-49
- Wostmann B. Indications for removable partial dentures: a literature review. Int J Prosthodont. 2005 Mar-Apr; 18(2):139-45
- McKenna et al The impact of rehabilitation using removable partial dentures and functionally orientated treatment on oral health-related quality of life: A randomised controlled clinical trial. Journal of Dentistry 2015 Vol.43(1):66-71
- Zitzmann et al. Strategic Considerations in treatment planning: deciding when to treat, extract or replace a questionable tooth. J Prosthet Dent. 2010 104(2):80-91
- Tada et al. Multifactorial risk assessment for survival of abutments of removable partial dentures based on practice-based longitudinal study. J Dent 41 (2013) 1175-1180
- Tallgren A.The continuing reduction of the residual alveolar ridges in completed denture wearers: a mixed-longitudinal study covering 25 years. J Prothet Dent 1972 Feb; 27(2):120-32
- Van Kampen FM. Masticatory function with implant-supported over-dentures. J Dent Res 2004 Sep; 83(9):708-11
- Wismeijer D. Multicentre prospective evaluation of implant-assisted mandibular bilateral distal extension removable partial dentures: Patient Satisfaction. Clin Oral Impl Res 24,2013,20-27
- J Feine, GE Carlsson et al. The McGill consensus statement on over-dentures. Gerodontology 2002 Jul 19(1):3-4
- Timmerman R, Stoker GT, Wismeijer D, Oosterveld P, Vermeeren JI, Van Waas MA. An eight-year follow-up to a randomised clinical trial of participant satisfaction with three types of mandibular implant-retained over-dentures. J Dent Res 2004 Aug; 83(8):630-3
- Semper W, Heberer S, Nelson K. Retrospective analysis of bar-retained dentures with cantilever extension: marginal bone level changes around dental implants over time. Int J Oral Maxillofac Implants. 2010 Mar-Apr; 25(2): 385-93
- Gallucci GO, Morton D; Weber HP Loading protocols for dental implants in edentulous patients. IJOMI 2009; 24(Suppl)132-146
- Kreisler M. Residual ridge resorption in the edentulous maxilla in patients with implant-supported mandibular over-dentures: an eight-year retrospective study. Int J Prosthodont 2003 May-Jun; 16(3):295-300
- Papadimitriou DE, Salari S, Gannam C, Gallucci GO, Friedland B. Implant-prosthodontic classification of the edentulous jaw for treatment planning with fixed rehabilitations. Int J Prosthodont.2014 Jul-Aug; 27(4):320-7
- Shamiri RA, Atieh MA Mandibular Kennedy Class 1 implant-tooth-borne removable partial denture: a systemic review. J Oral Rehabil 2010 Mar; 37(3): 225-34
- Stone AA, Schwartz JE, Broderick JE, Deaton A. A snapshot of the age distribution of psychological well-being in the United States. Proc Natl Acad Sci USA 2010 107(22) 9985-90
CPD responses closed
The CPD quiz for this article is now closed. Please check the listings for the current quizzeslistings


Comments are closed here.