Comprehensive case management
Not all cases are as straightforward as they may seem. The heavily restored dentition requires a careful, comprehensive assessment if the best treatment plan is to be arrived at
The following case reports on a patient initially referred for dental implant rehabilitation of posterior segments who, following comprehensive planning, elected for an entirely different treatment option.
The case
The patient was a 60-year-old female with a heavily restored upper and lower dentition. She was referred
for possible implant replacement of upper and lower posterior dentition.
Previous dental history
She was a regular attender with significant restorative care over her lifetime, most recently restorations and tooth loss required as teeth have failed due to loss of tooth structure.
Last treatment was fabrication of a new upper p/- chrome and RCT of lower 6s following crown loss.
Medical history
Slightly elevated blood pressure, controlled, otherwise clear.
Patient requirements/goals
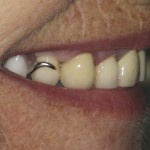
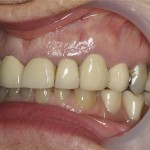
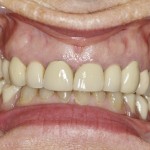
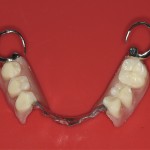
- Aesthetics was the highest priority. She disliked the spaces in the upper and lower posterior segments as well as visible clasps of upper chrome (Fig 1).
- Longevity and planning for future problems was important.
- She would also like to improve function.
Patient assessment
Extra-oral
Soft tissue assessment – no abnormalities detected.
Smile line – medium/high, showing gingival margins during a wide smile.
Intra-oral
Soft tissue assessment – no abnormalities detected.
Teeth present:
7__4321 – 12345_7
76__321 – 123__67
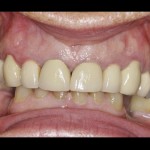
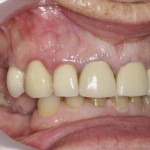
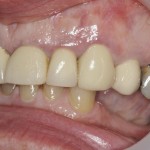
(Figs 2-4)
Restorative status and prognosis of remaining teeth:
Maxillae
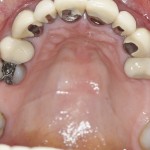
Eleven teeth remain, having had premolars on either side previously removed. Of the 11 remaining teeth, all of them are restored, with the eight upper front teeth having full coverage crowns (which have apparently been present for about 20 years). Three of these have root canal treatment and posts. The root fillings are all inadequate, with short posts.
No significant periapical pathology. A number of the crowns do not fit the underlying teeth, with the possibility that secondary dental decay is ingressing. The three root-filled teeth are sufficiently heavily restored that further treatment is unlikely and they are likely to be lost in the future.
The remaining back teeth on both sides, while again heavily restored, do appear sound at this time. There are no immediate dental restorative needs in the upper arch, just the concern that, as and when problems occur with the crowns in the upper front teeth, these teeth will be lost (Fig 5).
Mandible
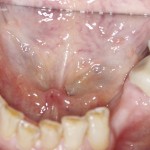
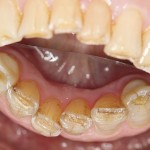
Ten teeth remain, again having lost premolars on either side. The lower six remaining front teeth, other than being slightly discoloured, are intact with minimal restoration and good prognosis. The second molars on either side have direct placement silver amalgam restorations, but are otherwise sound with good prognosis.
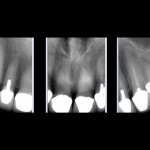
The first molars on either side recently had temporary crowns placed following root canal treatment. Radiographs show incomplete root canal fillings and insufficient tooth structure for predictable re-restoration (Fig 6).
- Visible clasp from existing denture
- At presentation
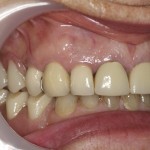
- Right lateral view
- Left lateral view
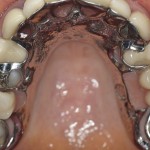
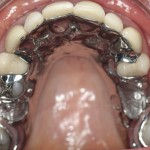
- Upper full arch mirror view
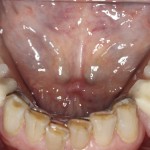
- Lower full arch mirror view
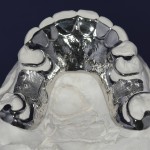
- Existing removable restorations
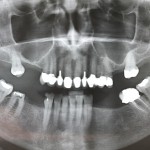
- OPG
- Radiographs of upper anteriors
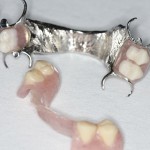
Existing removable restorations
The upper denture is a cobalt chrome reinforced denture with a palatal strap and visible buccal clasping. In the lower, there is a temporary all-acrylic denture (Fig 7).
Periodontal condition
BPE
1/1/1
0/2/1
Full chart not required.
Oral hygiene was fair, some areas of supra and subgingival plaque deposits. OHI practical required for effective plaque removal.
Occlusal assessment
TMJ healthy – full range of motion and no pain on loading.
Centric relation – first point of contact UL7 /LL7 and less than 1mm vertical slide to centric occlusion.
Guidance – group function on both sides with non working side interferences on both lower 7s.
Interarch spacing – limited above roots of lower 6s.
No evidence of significant parafunction.
Aesthetics
Medium/high smile line showing gingival margins of all upper anterior crowns and clasps of p/- chrome.
Unaesthetic old PFM crowns, poor width/length ratio, unaesthetic margins.
Lower spacing evident.
Staining and colour mismatch from restorations to remaining tooth structure.
Radiographic assessment
OPG – no non-dental issues, assessment of vertical bone height for possible implant placement suggest favourable situation in the lower arch with the need for bilateral sinus augmentation in the upper. (Fig 8 – OPG).
Periapical radiographs – upper anterior dentition heavily restored with root canal fillings, posts and crowns on teeth, no significant apical pathology (Fig 9 – periapical radiographs).
Diagnosis
Reduced aesthetics and function as a result of repeat restoration and tooth loss in a heavily restored dentition, with a high likelihood of further tooth loss, especially in the lower posterior and upper anterior sextants.
Discussion/treatment options
The patient was initially referred for possible implant replacement of missing posterior teeth in both arches. Initial assessment would suggest this as a reasonable and predictable way of restoring the posterior sextants to full function, with good bone height available in the lower and predictable augmentation likely in the upper.
Critical in any case assessment, however, is the overall assessment of the full mouth in order to predict, as far as possible, where problems will next occur and how they can be managed within the context of the planned treatment. This is never more important than when considering dental implants.
However it is managed, dental implant treatment is a costly process, financially and in terms of what patients may have to endure. It is important that, if we can predict that more implants are likely, the patient is made aware of this at the outset of treatment. Often a patient will stretch themselves for the treatment they have been told they need, but be unable to rise to additional complex treatment in the future.
Therefore, we need to look to the evidence available in order to predict what may happen to a heavily restored dentition. With this information, the patient is then much better informed and able to make the right decision about their care. In addition, as clinicians we are much better able to manage a situation if we have predicted and explained it in advance.
In compiling the treatment plan, advice on evidence-based prognosis and treatment outcomes was sought from specialist clinicians in prosthodontics, oral and maxillofacial surgery and endodontics.
With this particular case, the restorations most at risk of future failure are the upper post crowns. Due to the proximity of a number of post crown restorations, failure of any one would result in a significant challenge:
- Tooth loss will result in unaesthetic apical migration of the gingival margin.
- Fixed bridgework is unpredictable due to lack of structural integrity of adjacent teeth.
- Lifting a flap for implant placement, in the upper anterior sextant, will likely result in exposure of the crown margins on adjacent teeth. Restoration of these teeth to manage this would again be unpredictable due to lack of ferrule and structural integrity.
- Were it either of the lateral incisors that was lost, implant placement would be in a less than ideal strategic position, given that future tooth loss is likely.
Discussing the situation with the patient involves presenting the information in such a way that they can balance their wishes, what is possible and what is affordable both now and in the future.
In this case, we established that to resolve the original concerns, a minimum of two implants would be required in the upper arch and four in the lower.
Multidisciplinary planning suggests that additional treatment as problems arise in the upper would likely result in an additional two to four implants carried out in a “piecemeal” approach on an “as required” basis.
Many patients are happy to accept this and proceed as they originally intended. Here, however, the patient felt that their previous experiences and our observations meant further treatment would be highly likely and that they could not, and did not wish to, afford piecemeal implant dentistry.
The patient was willing to compromise their criteria to accept “removable” rather than “fixed” restorations if their other wishes could be achieved.
We therefore looked to provision of removable chrome reinforced partial dentures, designed in such a way as to achieve as many of the patients original wishes as possible as well as managing predicted future problems.
Agreed treatment:
Upper arch
Using a modified RPI (rest/plate/i-bar) system (Equipoise System), we were able to design an upper removable partial denture that did not show any of the metal clasping which had been bothering the patient. In addition, by opening the occluso-vertical dimension, in centric relation, it was possible to provide an anterior chrome bite platform that would both limit functional and para-functional forces on the existing post crowns while providing support for possible future tooth addition as and when required.
Lower arch
A “rotation” type chrome was fabricated to rest on composite additions to the lingual of the lower anteriors and within distal undercuts. The interocclusal space was limited over the remaining roots of the first molars, deeming them unsuitable as potential overdenture abutments, and these were therefore removed three months before restoration fabrication.
During treatment, the patient was instructed on optimal oral hygiene for the existing and planned restorations.
Treatment progression
Figs 10-18.
- Left lateral completed case
- Right lateral completed case
- Upper fitted
- Upper and lower chromes fitted
- Try-in of Equipoise framework
- Upper Equipoise framework
- Lower rotational denture fitted
- Completed lower rotational chrome
- Composite rests lingually on lower canines
Conclusion
A case has been presented demonstrating comprehensive, multidisciplinary, treatment planning as a result of which the patient chose a different treatment option from that which they had originally intended.
Planning advanced restorative dental care, in an already heavily restored dentition, is a complex and challenging process. If predicable results and patient satisfaction are to be achieved, then informing patients fully of all potential outcomes and possible future complications is essential at the outset.
About the authors
This article was submitted by Edinburgh Dental Specialists.
References
References available by request, email Tele-dentist@edinburghdentist.com for more information.
Verifiable CPD Questions
AIMS AND OBJECTIVES
- To understand the process of comprehensive case evaluation
- To appreciate the role of evidence based dentistry in case assessment
- To appreciate that dental implants are not always the best solution for tooth replacement
- To show that, integral to any comprehensive treatment plan, should be a prognosis not only for the planned restorations, but also the existing dentition.
LEARNING OUTCOMES
- To appreciate that comprehensive case assessment is a complicated process, bringing together not only the patient’s wishes and budgetary restraints, but also balancing these with knowledge of evidence-based treatment outcomes across a number of specialities
- To understand that a patient’s decision on the treatment they choose to have is dependent on the clear presentation of information in a way that is sympathetic to their current and future dental needs.
EXAMPLE QUESTION
1. What are the important aspects of a full case assessment?
a. Understanding the patient’s expectations
b. A full medical and dental history
c. Presenting all possible options in a clear understandable format
d. Predicting the potential future problems and how they
may be managed
e. All of the above.
Submit your answers listings

Comments are closed here.